Psychiatry-Cloud was built by practicing clinicians who understand the importance of an intuitive, intelligent EHR. Designed for psychiatry, our templates cut through the daily grind—delivering clarity, accuracy, and more room to focus on patients. And context collected by AI agents, threaded throughout every care touchpoint, reduces handoffs, re-entry, and missed details across the chart.
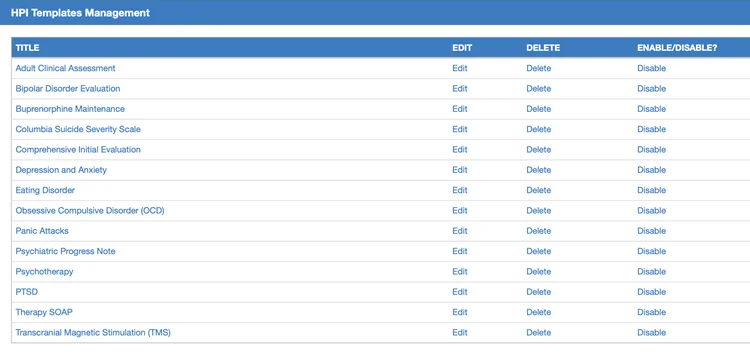
No two visits look the same—and your templates should reflect that. Psychiatry-Cloud offers documentation options for every stage of mental health care. Our system adjusts to each unique circumstance while keeping every chart consistent, accurate, and ready for clinical, billing, and compliance needs.
for structured histories that fit naturally into your chart
that captures new-patient details with clarity
for consistent follow-ups
built for everyday encounters
that supports psychiatrists, psychologists, and therapists
designed for shared sessions, co-signing, and coordinated care
Templates are only part of the solution. Psychiatry-Cloud’s intelligent platform levels up your note workflows with AI features like:
Our AI is intentional, built into the core of our platform, and made to help you reclaim your day. Practice management agents work quietly in the background, giving you clean, context-rich notes without adding more steps to your workflow.
Fill out the form below to request a personalized demo.